The following article appears in the Summer 2020 issue of Third & Broadway magazine, scheduled for delivery this month.

When Ed Zuroweste was a student at Transylvania University some 50 years ago, he’d harvest tobacco just outside Lexington before the school year kicked off.
Cutting tobacco under the blazing August sun in Kentucky isn’t what you’d call a pleasant summer job. It’s backbreaking labor.
Zuroweste, who toiled alongside migrants in those burley fields, went on to graduate in 1971 and then became a medical doctor — one who has dedicated his career to helping farmworkers who travel with the growing seasons and work hard for little pay.
Early on, just after he opened a clinic in rural Pennsylvania, Zuroweste saw a patient who happened to be a public health nurse serving more than a thousand migrants who’d travel to the area as apples, peaches and cherries ripened on the branches of orchard trees. After a few months they’d move on, maybe head up north to pick blueberries.
“I told her I speak Spanish and if she needed any help, let me know.” She did.
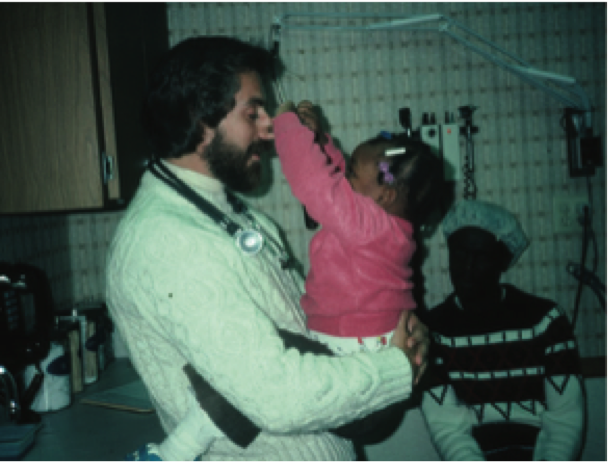
After a while, Zuroweste noticed many of his patients weren’t returning for follow-ups. Turns out, it was because he kept daytime office hours and they had to work the orchards all day. So in 1980, he started a nighttime clinic for them. “It really brought me back to my roots, and I felt very comfortable with the population,” said Zuroweste, who not only harvested tobacco but also grew up on a farm. “I could relate to them.”
(He probably wouldn’t have spoken Spanish had he and a Transy fraternity brother not ventured off to Mexico for their first year of medical school — he eventually graduated from the University of Cincinnati College of Medicine.)
In the mid ’80s, Zuroweste attended a national conference where he helped establish the Migrant Clinicians Network and became its founding medical director.
The group helps ensure migrants have a network where they can receive continuous care. Zuroweste was well aware of this problem as a physician in Pennsylvania, where he might, for instance, get patients’ diabetes under control — but they’d leave after a few months and return the next year with a worsened condition from lack of care in the interim.
The MCN also facilitates research and helps health care workers across the country coordinate efforts so they aren’t reinventing the wheel every time a new challenge arises. “Our organization has always been adaptable,” he said. “Whatever the issues are, we have to adapt to those quickly.”
One of these issues is the coronavirus. “When COVID came up it was in our wheelhouse at the Migrant Clinicians Network because we’d worked with things like this in the past.”
Zuroweste, who also is an assistant professor of medicine at Johns Hopkins School of Medicine, specifically has extensive experience with infectious diseases. He served the World Health Organization as a special medical consultant during the H1N1 pandemic and an African Ebola outbreak six years ago, when he used his Spanish to help train 200 Cuban physicians for a treatment center. Zuroweste now runs a tuberculosis clinic and is the TB medical consultant for the state of Pennsylvania’s Department of Health.

When COVID-19 struck, he and other MCN members quickly published informational materials and produced webcasts for migrants and those who treat them.
Because they’re part of our food production system, these laborers are considered essential workers, and as with hospital employees, they must ply their trade in a risky environment. Migrants often live in communal settings, travel by bus and work side by side (especially in packing houses). Also, if they’re undocumented they may be hesitant to seek help — or they may miss essential notices because of a language barrier.
“What we’re finding is there’s a huge number of infected farmworkers right now,” Zuroweste said.
That community health clinic he started has received a federal grant to handle migrant farmworker health care for the entire state of Pennsylvania. Challenges the clinic faces during COVID-19 range from the obvious, such as how to test migrants, to the not-so-obvious, like will wearing masks in the field contribute to heat stroke?
Handling such complexity and adapting to rapidly changing circumstances are skills fostered by the broad-based liberal arts education Zuroweste got at Transylvania — where he was pre-med, president of Delta Sigma Phi and studied a variety of subjects.
He credits the school with making him a better physician than he would have been with just a strict science background. “I think it’s really important to have a broad base of knowledge if you’re going into medicine,” he said.
Knowing your way around a tobacco barn might come in handy too.

